There is no escaping modern technology in medical practice today and digital health is no exception. In fact, research suggests some digital health solutions can be as impactful in the management of some diseases as a medication. Thus, the term: “software as a drug.”
We’re in the embryonic phase of realizing the promise of well-researched, clinically-validated digital health solutions. This includes employing clinical and behavioral models to develop process and clinical outcome measures during rigorous clinical trials. It also includes testing user experience (patients and providers) and then iterating the digital health solutions constantly based on feedback and rapidly evolving advances in disease management and technology capabilities.
Digital Health Mechanisms of Action
When we discuss a pharmaceutical or drug, we discuss the mechanisms of action. We can and should raise the same questions about digital health solutions and discuss the synergy between medications and other aspects of disease management. We should explore how the digital health solutions amplify the healthcare provider’s recommended treatment plan. We also need to ask how the digital health solutions coach the user to adhere to their medication regimen, make healthier lifestyle choices and monitor daily self-care. All are important in the case of managing diabetes.
Lastly, if software or a digital health solution will be as impactful on care as a pharmaceutical, it must also enable the transfer and utilization of data by the user and their provider. With this valuable data in hand, and as partners in care, the user (patient) and provider can continuously adjust the treatment plan.
Data Transforms into Applicable Information
Data can be defined as facts collected for analysis. Alone data has limited intrinsic meaning. Information, on the other hand, refers to items learned about something or someone. Information can convey significant insights about persons and events. Digital health solutions have the potential to collect massive amounts of data, but unless it is usable information upon which actions or disease treatment changes can be made, it’s not clinically valuable. As a physician who cares for people with diabetes, it is critical that I and the people I care for have access to usable and applicable information.
Allow me to make my point.
People with type 2 diabetes are often told by their healthcare provider to check their blood glucose with their meter every morning prior to eating (fasting) but then aren’t encouraged to check other times of the day, including before and after meals, etc. This case illustrates the challenge of collecting solely fasting glucose levels.
A person with type 2 diabetes came to see me for an initial visit. He regularly checks his blood glucose fasting at 7:30 am. In fact, he proudly showed me his records with 365 blood glucose results – all within a similar range. He was never told to check his glucose other times of the day to learn how food and activity might affect his glucose levels. So in essence we had lots of data, but it was of minimal use to adjust his diabetes management plan.
Conversely, less data that is collected wisely can become applicable information. For example, one of my patients, who has type 2 diabetes, provides me with glucose results from a mobile app he is using. I observe a blood glucose result of 153 mg/dL recorded at 10:52 am and another data point, a glucose of 89 mg/dL two hours earlier with data that he consumed 45 grams of carbohydrates at breakfast and took 8 units of insulin. This additional data paints a more complete picture of a specific time of day and becomes more applicable information with which I’m able to help Mr. Jones.
Unless people with diabetes are provided with guidance on when to check their glucose levels (data) intelligently they and their provider will not have data from which to review and revise their treatment plan. Even more importantly, their data can be put to good use by themselves and their healthcare provider if they’re using a digital health solution that offers real time feedback and actions to, for example, treat a low blood glucose or prevent a glucose rise.
Dense Data vs. Sparse Data
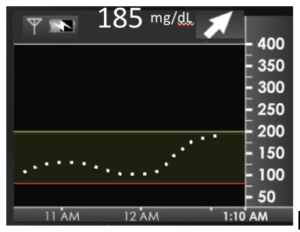
Taking this point one step further, let’s consider what data science experts call “dense data” vs. “sparse data.” In the image below (left), you see a tracing from a Continuous Glucose Monitor (CGM). It contains many data points – a result every 5 minutes. From this vast data recorded day after day and observable in various profiles, the patient and healthcare provider can see that this person’s glucose level starts to rise after midnight. We can impute the time that the user ate a midnight snack. The density of this CGM data makes it quite informative to observe glucose patterns day after day.
On the converse, consider the example of sparse data in the figure to the right. This is far fewer glucose data points, perhaps as few as 3 to 5 per week in a person who does a minimum of blood glucose checking with a meter.
Adding More Data Can Paint Context
The addition of more types of data can help the user and healthcare provider paint context and provide value as more actionable information. Continuing with the example of diabetes, digital health solutions should collect lifestyle data including medication doses and food intake with types, preparation and amounts consumed; and the timing and amount of physical activity.
But there must be a balance. The collection should not be overly intrusive. People with diabetes don’t want to spend hours collecting and imputing data. Digital health solutions can relieve some of this burden with an integrated or connected glucose meter, activity tracker and food bar code scanner. And as noted, the more the provider uses the patient’s data to make changes in the treatment plan and demonstrate the value of this data to the patient, the more they are likely to take the time to collect it and share it in a meaningful way.
Optimize Patient/User Engagement
The more easily this valuable data can be collected and enhance and reward user engagement, the better. However, user engagement, both initially and ongoing, can be a significant challenge. In digital health, engagement can be defined as the frequency of interactions the user has with the mobile app.
The right level of engagement for one person and their disease management can be very different from the next. Clinicians must learn to strike a balance with patients. The patient and the provider must gain sufficient data and feedback to make the app valuable without being burdensome. Patients and their providers may need to set different goals with the digital health solution at different times along the course of managing the chronic disease. These decisions can be part of the shared-decision making process.
A Final Thought
Einstein said “If you give me 60 minutes to solve a problem, I will spend 55 minutes thinking about the problem and 5 minutes working on the solution.” Technology can do many things, but we must develop solutions with a deep understanding of the complexities of the problem. We don’t need more data points, we need more applicable and actionable information.