Estimates show that people with diabetes have contact with their healthcare professionals only every 3 or 4 months at the most. The rest of the time they care for and manage their diabetes themselves. In fact, it is estimated that 95% of diabetes management is patient self-management.1
Self-management means that people themselves make decisions about how they will manage their lives and conditions within the context of other goals, priorities, health issues, and family demands. Research shows that through effective self-management, people with diabetes can improve their quality of life and reduce their risk of developing complications or comorbidities. Self-care can also help people reduce hospital admissions and readmissions or even reduce length of stay for a hospital visit.2
Understanding Success Factors for Self-Management
The increasing use of technology-enabled solutions for health management presents opportunities to improve patient self-management among individuals living with type 2 diabetes. Research has found that despite promising evidence, people typically stop using web-based solutions because of the burden of data entry, hidden costs, loss of interest, lifestyle practices, or lack of comprehensive solution features. Analyses generally tend to focus on effectiveness or impact and fail to evaluate the nuanced variables that may contribute to outcome success or failure, yet an understanding of those nuanced factors is crucial because evidence suggests a direct correlation between A1C improvements and better self-management. Based on Welldoc published studies that have analyzed success factors in the use of technology to improve diabetes self-management, five major areas of focus affect the effectiveness of self-management programs.
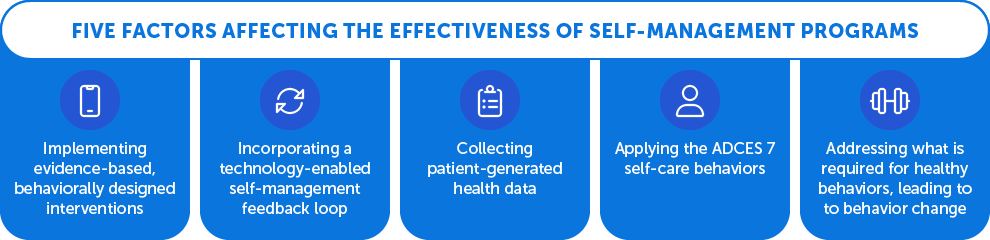
- Implementing evidence-based, behaviorally designed interventions to improve the reach of—and access to—diabetes self-management education and ongoing support
- Incorporating a technology-enabled self-management feedback loop that connects people with their healthcare teams by using two-way communication. Direct communication with healthcare providers has been shown to improve outcomes and facilitate engagement.3
- Collecting patient-generated health data, analyzing it for patterns and signals, and then interpreting the results and conveying them to the participant in a meaningful way so the person can become empowered to proactively take action on his or her health decisions.
- Applying the AADE 7 Self-Care Behaviors after customized and tailored education, which completes the feedback loop. Studies show that A1C improves when participants document their own health data and review data online in real time so they can receive in-the-moment digital coaching.
- Addressing what is required for behavior change as a core focus of better self-management—especially when it comes to the use of technology.
Implementing the Feedback Loop
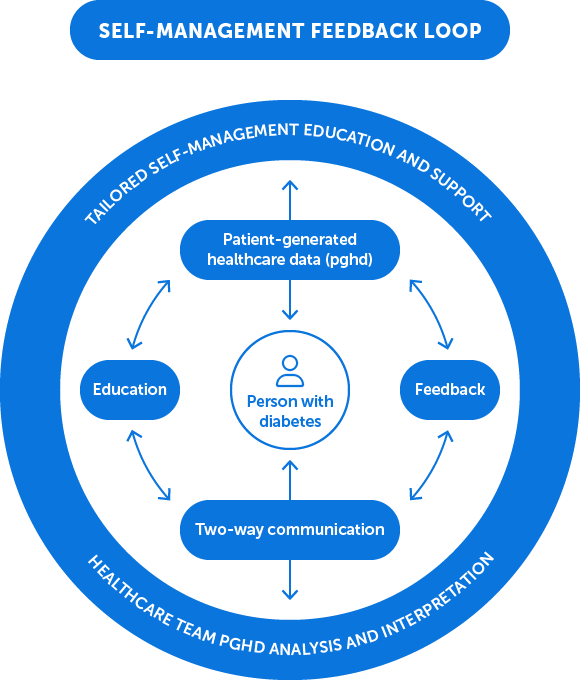
A technology-enabled feedback loop supports an informed and activated patient as well as a more-prepared, proactive healthcare team. The feedback loop incorporates monitoring, interpretation of data, adjustment of treatment, and the communication of tailored advice and then repetition of the cycle as required elements of condition management.
In a poster presented at a Diabetes Technology Society meeting, the coauthors found that the most-effective interventions incorporated all of the components of a technology-enabled self-management feedback loop that (1) connects people with diabetes and their healthcare team by using two-way communication, (2) analyzes patient-generated health data, (3) provides tailored education, and (4) sends individualized feedback.
A separate poster presented at AADE18 explored the role of the educator as a digital champion by leading the healthcare team in a population management, technology-enabled, team-based diabetes self-management education and support approach.
In the model explored in the poster, the authors propose that the educator lead the healthcare team and use the resulting patient-generated health data in a complete feedback loop to inform timely treatment and care plan optimization through shared decision making that is designed to achieve improved metabolic outcomes and quality of life.⁴
Enable Behavior Change in Self-Management
In another study that points to the behavioral factors that contribute to program success or failure and that is entitled “A Mobile App to Improve Self-Management of Individuals With Type 2 Diabetes: Qualitative Realist Evaluation,” the authors evaluated Welldoc’s BlueStar® for diabetes management so as to identify key combinations of variables and mechanisms of action that explain (1) for whom the solution worked best and (2) in what circumstances.
The study authors—who represented the Women’s College Hospital Institute for Health System Solutions and Virtual Care, the Institute of Health Policy, Management and Evaluation at the University of Toronto, the Knowledge Institute, and the American Academy of Nursing—found that a number of factors determined engagement levels. Those factors included self-efficacy, competing priorities, previous behavior change, and willingness on the part of individuals to engage with web-based solutions. Together the factors contributed to both engagement levels and impact on clinical outcomes.
Key Findings
The study5 found distinct patient characteristics and associated levels of self-efficacy; the groups consisted of:
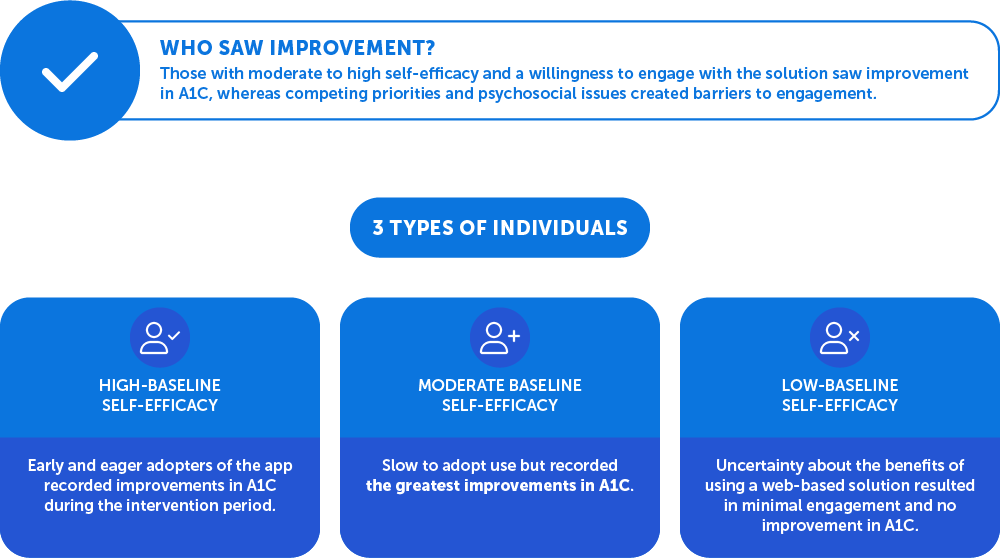
- Those who saw improvements: Self-efficacy and willingness to engage with the solution facilitated improvement in A1C, whereas competing priorities and psychosocial issues created barriers to engagement.
- Those with high baselines: Individuals with high-baseline self-efficacy who were motivated, who took ownership for their actions, and who prioritized diabetes management were early and eager adopters of the app and recorded improvements in A1C during the intervention period.
- Those with moderate baselines: Individuals with moderate baseline self-efficacy and no competing priorities and who identified gaps in understanding the ways their actions influence their health were slow to adopt use but recorded the greatest improvements in A1C.
- Those who had low baselines: Those with low-baseline self-efficacy had earlier identified a range of psychosocial issues and competing priorities. They were uncertain about the benefits of using a web-based solution to support self-management, which ultimately resulted in minimal engagement and no improvement in A1C.
References
- Funnell MM, Anderson RM. The problem with compliance in diabetes. JAMA. 2000;13:1709.
- American Diabetes Association. Diabetes self-management education; https://www.professional.diabetes.org/diabetes-self-management-education. Accessed September 21, 2021.
- Bonoto BC, de Araújo VE, Godói IP, et al. Efficacy of mobile apps to support the care of patients with diabetes mellitus: a systematic review and meta-analysis of randomized controlled trials. JMIR Mhealth Uhealth. 2017;5:e4. 24; Toma T, Athanasiou T, Harling L, et al. Online social networking services in the management of patients with diabetes mellitus: systematic review and meta-analysis of randomised controlled trials. Diabetes Res Clin Pract. 2014;106:200-211.
- Greenwood, D., Gee, P., Fatkin, K., & Peeples, M. 2017 A Systematic Review of Reviews Evaluating Technology Enabled Diabetes Self-Management Education and Support. JDST. e-published May 31
- Twenty-six interviews (14 baseline, 12 follow-up) were completed with 16 participants with type 2 diabetes mellitus, and the following three key groups emerged: the easiest fit, the best fit, and those who failed to activate.
