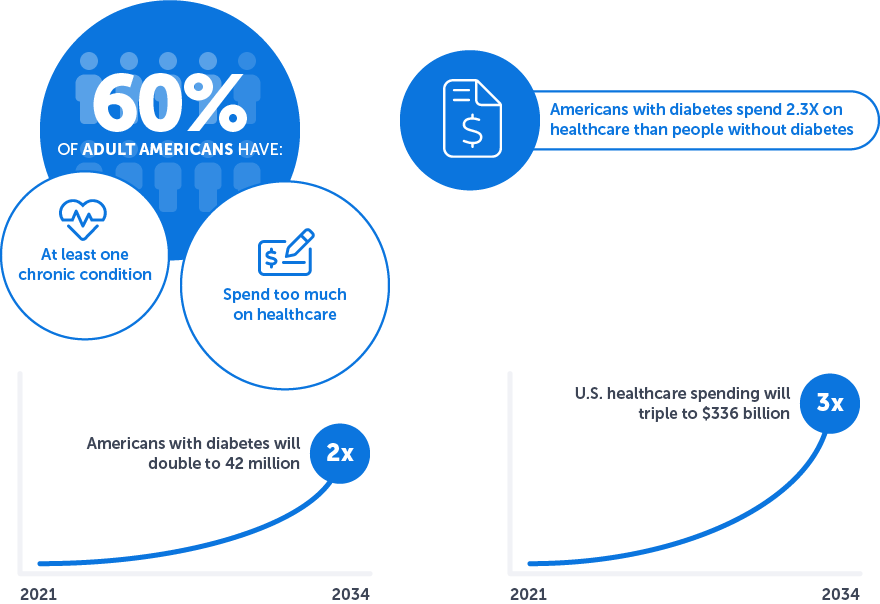
Research has shown that people with chronic conditions—about 60% of American adults—have at least one chronic condition and use a disproportionate amount of healthcare services, totaling hundreds of billions of dollars in healthcare spending every year.1 In fact, those at the highest end of the scale, with five or more conditions, represent about 12% of the US adult population, yet they account for a staggering 40% of healthcare spending.2
Increases in the number of people living longer with chronic conditions, coupled with rising healthcare expenditures, make the current trajectory unsustainable. Consider for a moment the cost of diabetes to the healthcare system. One estimate projects that by 2034, the number of people with diabetes is expected to double to 42 million and related healthcare spending will triple to $336 billion.3 The cost translates into average medical expenditures of $16,752 per year, of which about $9,601 is attributed to diabetes. On average, people with diagnosed diabetes have medical expenditures approximately 2.3 times higher than expenditures would be in the absence of diabetes.4
A Scalable Approach to Cost Savings and Outcomes
Many health plans are meeting this growing challenge by piloting and rolling out innovative strategies to reduce healthcare use and costs among this population. Care management programs aim to provide better care while reducing the costs of caring for the chronically ill, including costs associated with avoidable complications such as emergency room visits, hospitalizations, and readmissions.4
In a review of chronic care management programs,5 survey authors from Rand Corporation and sponsors from America’s Health Insurance Plans Foundation found that health plans are addressing member needs along the continuum of care. Their guidance is presented in the forms of various types of wellness programs and lifestyle management programs that are offered to members with chronic disease based on disease-state progression.
To better understand how holistic health plan strategies might affect outcomes, LifeScan and Welldoc initiated a large health plan digital health study undertaken to evaluate pre- and post-system use, A1C, trends in average blood glucose, incidence of hypoglycemia and hyperglycemia, medication adherence, healthcare utilization, comorbidities, medical utilization, and costs.
The study suggests that real-time availability of data-driven insights assists users and their own providers in improvements in glycemic control and in shifts to data-driven care. The use of intelligent monitoring engages members beyond just glucose testing to include lifestyle and psychosocial monitoring, to provide robust data for treatment optimization, and to lead to higher-quality engagements that may be the “active ingredient” in influencing clinical outcomes and reducing costs.

Research Key Findings
In a related poster presented by Aetna/CVS Health, Welldoc, and LifeScan at the ADCES20 Annual Meeting, the coauthors presented the results of a study of a population of commercial health plan members who represented typical type 2 diabetes members (health plan data analysis completed by Healthagen).
Engagement
- An average of 30 digital engagements per week was observed for those who activated and engaged, suggesting an effective mechanism to improve patient self-management of diabetes.
Utilization
- Diabetes-related and all-cause emergency room visits and costs decreased from baseline to follow-up.
- Reductions in diabetes-related costs were highest among members who began using OneTouch Reveal Plus with A1C above 8.
- Average pharmacy costs increased when compared with baseline, reflecting the increased usage of insulin and noninsulin drugs.

References
1,2 Mattke S, Mengistu T, Klautzer L, et a;. Rand Corporation, Improving Care for Chronic Conditions: Current Practices and Future Trends in Health Plan Programs, sponsored by America’s Health Insurance Plans Foundation. https://www.rand.org/pubs/research_reports/RR393.html.
3 Mattke S, Mengistu T, Klautzer L, et al. Improving Care for Chronic Conditions: Current Practices and Future Trends in Health Plan Programs. Rand Health Quarterly; https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5158283/.
4 American Diabetes Association, https://www.diabetes.org/resources/statistics/cost-diabetes.
5 Zhuo et al., 2012
